Dr. Saber’s Blog
Botox Treatment for Migraines: What You Need to Know
If you have suffered from migraine headaches or have lived with someone who has suffered migraine headaches, you know that a migraine is not just a worse-than-usual headache. A migraine is a wholly different beast. And it’s a beast that is very difficult to tame.
What’s a migraine?
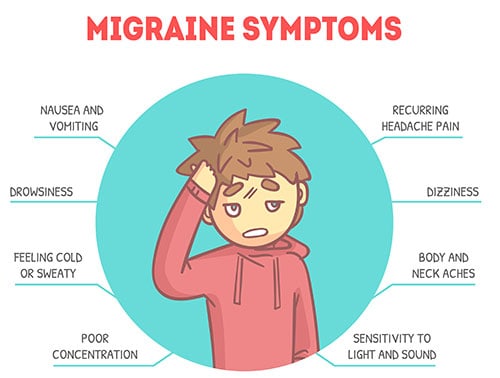
A migraine attack does, of course, involve a headache. But a migraine is also an incapacitating neurological disease with a wide range of symptoms, including visual disturbances, nausea and vomiting, dizziness, sensitivity to light, noises, and scents, and sometimes temporary weakness on one side. Episodes can last for hours, sometimes even for days.
According to the World Health Organization, migraines affect one in seven adults worldwide. In the United States, nearly 40 million Americans are beset by migraines. Of those 40 million victims, at least 28 million are female (this disparity is apparently due to women’s hormonal fluctuations).
How to diagnose a migraine
A migraine diagnosis is reached after a specialist (often a neurologist) reviews the patient’s medical history, the results of physical and neurological examinations, and the patient’s specific symptoms.
The symptoms of a migraine episode usually occur in four successive stages:
- The prodrome phase
- The migraine aura
- The migraine headache attack itself
- The postdrome headache
What’s a prodrome phase?
A day or so before a migraine the patient might notice subtle changes that serve as a warning of an incipient migraine attack. These prodromal symptoms might include:
- Mood changes, ranging from depression to euphoria
- Odd food cravings
- Neck pain
- Increased urination
- Frequent and uncontrollable yawning
What’s a migraine aura?
The components of a migraine aura may include visual phenomena, like seeing geometric shapes, patterns of bright spots, or flashes of light.
Other components of a migraine aura can be a brief loss of vision, a pins and needles sensation in an extremity, weakness, or numbness in the face or on one side of the body, or speech difficulty.
Many people have migraine without aura.
The migraine attack itself
The headache component of a migraine usually lasts between 4 and 72 hours unless treatment intervenes. The frequency of migraines varies widely from person to person. Chronic migraine is defined as at least 15 headache days per month, with at least eight of those headache days involving migraines. Episodic migraine is defined as less than 15 migraine days per month.
During the attack stage, the patient will experience severe pain, usually more prevalent on one side of their head. Migraine pain may throb or pulse; there will be heightened sensitivity to light, sound, and sometimes even the senses of smell and touch; nausea and consequent vomiting are frequent during an attack.
…a migraine is not just a worse-than-usual headache. A migraine is a wholly different beast.
The postdrome migraine
A migraine attack will leave its victim feeling drained, confused, and practically inert for about a day. However, some patients report feeling elated or euphoric. Any sudden movement might briefly bring the pain back.
What triggers migraines?
Occurrences related to the onset of a migraine include:
- Hormonal changes. Fluctuations in estrogen, such as those that occur before or during menstrual periods, pregnancy, and menopause, seem to trigger migraine attacks in many women. Logically enough, hormonal medications, such as oral contraceptives, can also bring on migraines.
- Alcohol, especially wine, and an excess of caffeine can also be related to migraines.
- It also seems clear that stress, whether domestic or occupational, can be a migraine trigger.
- Sensory stimuli, such as bright or flashing (strobe) lights, loud and/or sudden sounds, and strong smells, like perfume, paint, gasoline, or tobacco, trigger migraines in some people.
- Alterations in sleep patterns also appear to be connected with some migraines.
- Changes in the weather, accompanied by corresponding changes in barometric pressure, seem to be associated with migraines.
Migraine risk factors
Several factors serve to increase the likelihood of migraines. These include:
Inheritance: A patient with a family history of migraines is more likely to suffer migraines themself.
Age: Migraines generally first occur during adolescence. They tend to peak during a patient’s 30s and then, during subsequent years, the attacks tend to gradually become both less severe and less frequent.
How to treat migraine headaches
As evidenced above, the myriad potential causes are opaque, mysterious, and widely varied. Ditto for the panoply of treatment options for migraines.
Migraine treatments are categorized as either acute or preventative. Acute treatments are interventions during a migraine episode, designed to stop, or at least abate, the ongoing symptoms. Acute migraine treatments include over-the-counter medications and prescription drugs, some of which were originally designed to reduce blood pressure, decrease depression, or eliminate seizures.
Preventative migraine treatments are used regularly, irrespective of migraine episodes, and are meant to reduce the frequency, severity, and duration of attacks, all before the attacks occur. Preventative treatments include lifestyle changes designed to reduce stress, biofeedback, dietary protocols, prescription migraine medications, avoidance of triggers, behavioral therapy, and physical therapy.
CALL (818) 770-7050 OR CLICK HERE TO SCHEDULE ONLINE
Botox injections as migraine treatment
Another preventative treatment is multiple and repeated injections of poison. That is to say onabotulinum toxin – commonly known as Botox-A. It’s derived directly from clostridium botulinum, which is the same substance that causes the deadly disease of botulism.
Botox has been justifiably called the Swiss Army knife of medications, because it is currently being used to treat an impressively wide array of medical conditions, such as:
- Underarm sweating, a use approved by the Food and Drug Administration (FDA)
- An overactive bladder (FDA approved)
- Crossed eyes (FDA approved)
- Depression (not FDA approved)
- Abnormal heartbeat (not FDA approved)
- Severely cold hands (not FDA approved)
- Neck spasms (FDA approved)
- Various sexual conditions (not FDA approved)
- And, in 2010, the FDA approved Botox for chronic migraine headaches.
By the way, those non-FDA-approved uses of Botox are usually legitimate and ethical healthcare practices. Once a drug has been approved by the FDA for one use, doctors are free to use their professional discretion to use it in other applications (called “off-label use”).
How does Botox work for migraine headaches?
We need to again emphasize that the etiology of migraine headaches is difficult to definitively pin down. It’s correspondingly difficult to clearly understand how migraine treatments work. When it comes to understanding how Botox as a treatment of chronic migraines works, the best-educated conjecture of headache specialists is that the use of Botox injections (as well as injections of a competitive neurotoxin known as Dysport) disable the nerve endings present in and around the injection sites.
During a migraine, the patient’s body releases substances called neurotransmitters and other molecules associated with pain. Botox apparently blocks the transmission of pain by partially paralyzing a local network of nerves. (Note that this Botox is the same substance that is used to eradicate wrinkles by creating muscle weakness in ground zero for wrinkles, i.e., the area between the eyes and above the nose.)
What are the side effects of Botox for migraines?
At the hands of an experienced medical doctor, side effects are very rare, but they can occur. Side effects include:
- Headache or flu-like symptoms
- Watering or dry eyes
- Drooping of an eyelid, eyebrow, or one side of the mouth
Very rarely, the toxin might spread into the patient’s system. A patient should seek medical advice immediately if any of the following occur:
- Vision problems
- Significant abnormal muscle weakness
- Trouble in speaking or swallowing
- Difficulty breathing
Does Botox really work for migraines?
Yes, it does. Multiple clinical trials have shown that Botox provides enough reduction in headache days and improves the quality of life to merit FDA approval as a treatment for chronic migraines. A subsequent large-scale two-year European study reported in June 2021 showed the impact of onabotulinumtoxin A treatment on health resource utilization.
Botox has been justifiably called the Swiss Army knife of medications…
In other words, the study was meant to reveal whether Botox/Dysport would reduce the number of hospitalizations and healthcare professional visits among patients with chronic migraine. The study also collected “health economic data,” which measured both the participants’ utilization of medical resources and their work productivity.
At the end of the two-year study, the patients (85% of whom were women) reported significantly fewer headache-related hospitalizations in the past three months than during the three months immediately before the study began. Reductions in the use of all health services for headache conditions were also reported.
Botox really is an effective treatment for chronic migraine.
Botox for Migraine FAQs
Q: How much does Botox for migraines cost?
A: The cost of Botox for the FDA-recommended dosage of 155 units costs between $300 and $600 for each comprehensive treatment. You would think since the treatment is FDA-approved it should be covered under most insurance plans. However, there is likely to be an insurance requirement that at least two other, less expensive, treatment modalities be tried first.
Q: Where do they inject Botox for migraines?
A: According to Allergan, the manufacturer of Botox, tiny amounts of Botox are injected into 31 sites located on the patient’s face, sides of the head, and neck. There is some pain associated with the injections, but the discomfort is usually brief and minor.
Botox injections for migraines are effective for about 12 weeks, so repeated injections are required. It is reported that successive sets of injections each tend to be more effective than the last, so that maximum benefit is achieved after three or four sets of injections.
Why Choose Saber Plastic Surgery for Botox injection treatment?
Dr. Sepideh Saber is an American Board of Plastic Surgery-certified plastic surgeon practicing in the greater Los Angeles area.
She graduated from Stanford University’s world-renowned medical school and did her plastic surgery residency at the equally lauded University of Southern California (USC). She then completed a fellowship at New York University (NYU) in the extremely challenging and delicate disciplines of hand surgery and microsurgery.
Dr. Saber offers a more sensitive, female perspective for patients of all ages, genders, and orientations. Former patients from all walks of life have praised not only their treatment outcomes but her caring, thoughtful approach to a wide array of appearance and health-related matters.
To request a consultation, call 877-205-4100 or schedule a consultation online.
Dr. Saber takes her patients’ safety very seriously. Her facility’s Covid-19 patient safety procedures exceed all CDC and World Health Organization recommendations. Masks are required in our office at all times during the coronavirus pandemic.
The practice of Dr. Saber is located in Encino, CA for patients throughout the Los Angeles area. We are also convenient to Woodland Hills, Sherman Oaks, Calabasas, Burbank, Glendale, Hidden Hills, Agoura Hills, Northridge, North Hollywood, Malibu, Topanga, Canoga Park, Reseda, Valley Glen, Chatsworth, West Hills, Winnetka, Universal City, Bel Air, Beverly Hills, Downtown Los Angeles, Silverlake, and Echo Park.
- Pregnancy After a <span>Mommy Makeover<span> - January 5, 2026
- Why Some Smart Moms Wait: Surprising Benefits of <span> Delaying Your Mommy Makeover <span> - December 23, 2025
- Lymphatic Massages After Mommy Makeover: <span>Finding Relief and Healing<span> - December 12, 2025